-
Encompass Health and BSA Health System host grand opening for new inpatient rehabilitation hospital in Amarillo
Read more: Encompass Health and BSA Health System host grand opening for new inpatient rehabilitation hospital in AmarilloThe hospital is expected to open to patients in November. AMARILLO, Texas, Nov. 6, 2025 – Today, Encompass Health, the nation’s largest owner and operator of inpatient rehabilitation hospitals, along with BSA Health System, the largest healthcare employer in the Texas Panhandle region, hosted a grand opening for Rehabilitation Hospital of Amarillo. The 50-bed inpatient…
-
BSA Health System launches life-saving ECMO services
Read more: BSA Health System launches life-saving ECMO servicesAMARILLO, Texas (October 10, 2025) — BSA Health System has launched a new Extracorporeal Membrane Oxygenation (ECMO) program, introducing advanced, life-saving technology that provides critical support for patients experiencing severe heart or lung failure. ECMO functions as a temporary artificial heart and lungs, giving a patient’s organs time to rest and heal. It is used…
-
Why Breast Cancer Screenings Matter: Amy’s Story
Read more: Why Breast Cancer Screenings Matter: Amy’s Story“I never thought it would happen to me. But one mammogram changed everything.” Like many women, Amy Rambo scheduled her annual mammogram at BSA Harrington Breast Center as part of her routine care. But in December 2024, that screening brought news she never imagined. While sitting in a restaurant with her husband, Amy opened her…
-
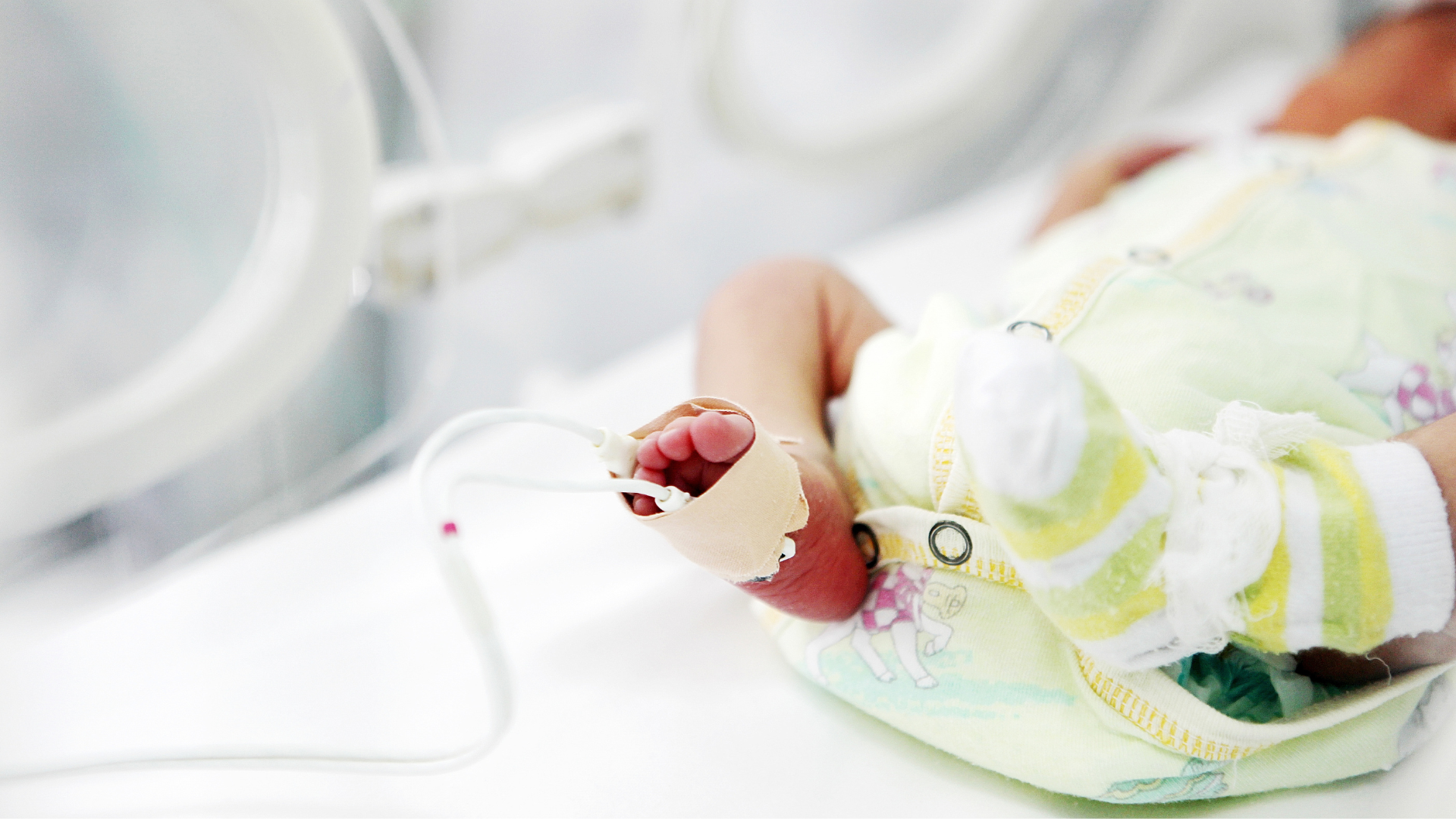
A Journey of Strength: One Family’s Story from the BSA NICU
Read more: A Journey of Strength: One Family’s Story from the BSA NICUThroughout NICU Awareness Month, we are honored to share stories that highlight the NICU journey. This month, we’re highlighting a local family whose baby boy spent his first days in the BSA Neonatal Intensive Care Unit. Their story reflects the challenges parents face, the support they receive and the joy that follows. An Unexpected StartWhat…
-
Healthy Lifestyle Choices to Lower Your Breast Cancer Risk
Read more: Healthy Lifestyle Choices to Lower Your Breast Cancer RiskDuring Breast Cancer Awareness Month, it’s a good time to think about steps you can take to protect your health. While not all risk factors can be controlled, healthy habits can lower your chance of developing certain cancers and other health problems. Small changes can make a big difference. Maintain a Healthy Weight Being at…
-
From Fear to Hope: A NICU Mom’s Story
Read more: From Fear to Hope: A NICU Mom’s StorySeptember is NICU Awareness Month, a time to recognize the strength of our tiniest patients and their families in the Neonatal Intensive Care Unit (NICU). This month, we share the story of Alexa Contreras, a NICU mom whose journey demonstrates the resilience that define the NICU experience. A Challenging BeginningAlexa’s journey to motherhood took an…
-
Answers to Common Breastfeeding Questions
Read more: Answers to Common Breastfeeding QuestionsExpecting and new mothers often have questions about the best ways to feed their newborns. We asked Tiffany Bateman, RN and board-certified lactation consultant at BSA Hospital, to share her insights on some of the most common breastfeeding questions. Which is better for my baby – formula or breast milk? Breast milk is considered the…
-
Encompass Health and BSA Health System announce joint venture to own and operate rehabilitation hospital in Amarillo, Texas
Read more: Encompass Health and BSA Health System announce joint venture to own and operate rehabilitation hospital in Amarillo, TexasBIRMINGHAM, Ala., and AMARILLO, Texas, August 15, 2025 – Encompass Health Corp. (NYSE: EHC), the nation’s largest owner and operator of inpatient rehabilitation hospitals, and BSA Health System, an affiliate of Ardent Health and the fourth largest employer in Amarillo, today announced a joint venture arrangement to own and operate a freestanding, 50-bed inpatient rehabilitation…
-
5 Essentials to Look for in a Childbirth Center
Read more: 5 Essentials to Look for in a Childbirth CenterChoosing the best childbirth center to welcome your baby into the world is a big decision, and let’s be honest—it can feel a bit overwhelming. Whether you’re searching for a hospital or a birthing center, it’s important to choose a facility that aligns with your birth plan and personal needs. From pain management options to…
-
What to do if … you have the flu
Read more: What to do if … you have the fluMany people believe flu season only lasts a few months, but it can stretch through seven months of the year. Learn tips on what to do if you think you may have the flu. What are symptoms of the flu? – Fever of 100.4 degrees Fahrenheit or higher – Chills – Cough – Sore throat …